- 首页 > 正文
透析患者使用盐皮质激素受体拮抗剂:疗效争议与研究新方向 | ERA大咖谈
发表时间:2025-08-19 16:00:34
编者按:在第62届欧洲肾脏协会年会上,加拿大麦克马斯特大学的Lonnie Pyne博士报告了其最新的系统评价和荟萃分析结果,该研究探讨了盐皮质激素受体拮抗剂(MRA)在需要透析的肾衰竭患者中的疗效。肾医线特邀Lonnie Pyne博士就此内容进行了深入分析。
肾医线:您的最新系统评价和荟萃分析聚焦于透析患者使用盐皮质激素受体拮抗剂的情况。从最新证据中,您观察到的最重要发现或趋势是什么?
Pyne博士:我们原本希望发现这类药物能降低心血管死亡率。但遗憾的是,与此前关于该主题的系统评价和荟萃分析结果相反,我们发现对于需要透析的肾衰竭患者,盐皮质激素受体拮抗剂并未降低心血管死亡风险,也未降低全因死亡率或心力衰竭住院率。从疗效来看,这类药物并无获益未显示出益处,反而带来了一些相关副作用,尤其是高钾血症发生率增加。我们将高钾血症定义为血钾≥6.5 mmol/L,其优势比约为1.5,即风险增加约50%;此外,男性乳房发育或乳房胀痛的发生率增加了3~3.5倍。而对于这一患者群体而言,盐皮质激素受体拮抗剂并未带来真正能抵消这些副作用的益处。
Nephrology On-line: Your updated systematic review and meta-analysis focus on mineralocorticoid receptor antagonists in dialysis patients. What are the most significant findings or trends you observed from the latest evidence?
Dr Pyne: We were hoping to find that they would lower cardiovascular mortality. Unfortunately, what we found was that in contrast to the prior systematic reviews and meta-analyses on this topic, mineralocorticoid receptor antagonists in patients with kidney failure requiring dialysis did not lower the rates of cardiovascular death, did not lower the rates of overall all-cause mortality, and did not lower the rates of heart failure hospitalization. So, in terms of efficacy, they were not found to be beneficial, and did have some relevant side effects, particularly increasing the rates of hyperkalemia. We defined hyperkalemia as potassium greater than or equal to 6.5. Odds ratio for that was about 1.5, so an approximately 50% increase, as well as a three to three-and-a-half times increase in the rate of gynecomastia or breast tenderness. So, some relevant side effects, but no really offsetting beneficial effects of mineralocorticoid receptor antagonists in this patient population.
肾医线:这些发现对当前肾衰竭透析患者的临床指南或治疗决策有何影响?
Pyne博士:至少在我的临床实践中,我并不会常规地对所有需要透析的终末期肾病患者使用盐皮质激素受体拮抗剂,临床实践指南中也未作此推荐。因此,这些发现与我的临床实践一致,即不常规推荐使用此类药物来降低心血管事件风险,同时也需考虑其显著的副作用。不过,对于存在其他适应证的患者(例如射血分数降低的心力衰竭患者),不应以此研究结果作为反对使用盐皮质激素受体拮抗剂的证据。这一结论仅针对未筛选的终末期肾病透析患者,我将继续保持不常规使用此类药物的临床实践。
Nephrology On-line: How do these findings influence current clinical guidelines or treatment decisions for patients with kidney failure on dialysis?
Dr Pyne: I think right now, at least in my own personal practice, I was not routinely using mineralocorticoid receptor antagonists for an unselected patient population with end-stage renal disease requiring dialysis, and nor was that something that was recommended in clinical practice guidelines. So, I think, in that sense, my own personal clinical practice would be pretty consistent, which is to say that they would not be recommended routinely to lower the risk of cardiovascular events, and also considering the important side effects profile there. Now, outside of that patient population, should they have another indication for mineralocorticoid receptor antagonists, if they have heart failure with reduced ejection fraction for example, I don't think this should be used as evidence to counteract that. This is merely saying, in an unselected patient population of end-stage renal disease requiring dialysis, I was not routinely using mineralocorticoid receptor antagonists and that will continue to be my practice.
肾医线:基于您的分析,该人群中盐皮质激素受体拮抗剂的安全性和有效性研究仍存在哪些空白?未来研究应优先关注哪些方向?
Pyne博士:我们的系统评价关注的是针对需要透析人群使用任何类型盐皮质激素受体拮抗剂(MRA)的随机对照试验。但我们发现,所有纳入的试验都仅使用了甾体类盐皮质激素受体拮抗剂。除了一项研究使用依普利酮外,其余均采用螺内酯 —— 这两种药物都属于甾体类 MRA。
在我看来,当前最明显的研究空白在于:非甾体类盐皮质激素受体拮抗剂的效果如何? 这类药物在透析患者中是否存在不同作用,是一个值得特别关注的领域。目前,至少在北美,可用的非甾体类MRA为非奈利酮,但它尚未获批用于需要透析的肾衰竭患者,这无疑是最关键的研究缺口之一。
此外,还有一些更重要的问题亟待解决:如何选择合适的临床终点?在需要透析的终末期肾病患者中,该如何定义 “心力衰竭住院”?我们是否需要对心血管终点进行更细致的分类?当前多数试验仅关注总体心血管死亡率,其中既包括心律失常、心源性猝死、心力衰竭等心脏事件,也混杂了心脏病发作、中风等血管事件。而 MRA 对这两类事件的影响是否存在差异,我认为值得深入探究。
Nephrology On-line: Based on your analysis, what are the remaining gaps in research regarding the safety and efficacy of mineralocorticoid receptor antagonists in this population, and what should future studies prioritize?
Dr Pyne: That's a great question. As mentioned, our systematic review was looking at randomized controlled trials of any type of mineralocorticoid receptor antagonists in people requiring dialysis. We only found trials using steroidal mineralocorticoid receptor antagonists. All of the studies, except for one, were of spironolactone. One was of eplerenone. Both spironolactone and eplerenone are steroidal mineralocorticoid receptor antagonists. So, to me, the most glaring gap would be what effect do non-steroidal mineralocorticoid receptor antagonists have? Whether or not there is a different effect in this patient population would be an area that I think would be of particular interest. Currently, at least in North America, the available non-steroidal mineralocorticoid receptor antagonist is finerenone but it is not approved for patients with kidney failure requiring dialysis. I think that would be one of the most relevant gaps. Then the bigger questions are what outcomes to use, how to define heart failure hospitalization in patients with end-stage disease requiring dialysis, and whether we need to be more narrow for our cardiovascular outcomes. Most of the trials looked at overall cardiovascular mortality, which includes cardiac events of arrhythmias and sudden cardiac death and heart failure, but also lumps vascular events in together, like heart attacks and strokes. Whether or not mineralocorticoid receptor antagonists affect those two types of events differently would, I think, be worth looking into.
报告概要
盐皮质激素受体拮抗剂在接受透析的肾衰竭患者中的应用:一项最新系统评价和荟萃分析
研究背景:透析患者心血管风险与MRA的应用争议
终末期肾病患者常伴随高发心血管事件,而盐皮质激素受体拮抗剂(MRAs)在慢性心力衰竭和慢性肾病(CKD)患者中已被证实可降低心血管风险。然而,这类药物在需要透析的肾衰竭患者中的疗效与安全性一直存在争议。
研究方法:纳入19项研究的全面证据整合
研究团队检索了截至2025年3月的MEDLINE、Embase等数据库,纳入19项随机对照试验(RCT),覆盖接受维持性透析(血液透析或腹膜透析)的成年患者,比较MRA(如螺内酯、依普利酮)与安慰剂/标准治疗的疗效与安全性。主要终点包括心血管死亡、心力衰竭住院、全因死亡,次要终点涉及高钾血症、男性乳房发育等不良反应。研究采用GRADE方法评估证据确定性,并通过随机效应模型分析异质性。
关键结果:MRA未带来生存获益,副作用显著
1.心血管与全因死亡无改善:
低偏倚风险研究显示,MRA组心血管死亡风险比(OR)为0.98(95%CI:0.80~1.20)(图1),全因死亡OR为0.97(0.84~1.21),均无统计学意义。高偏倚风险研究中,MRA虽显示心血管死亡风险降低(OR 0.33,0.17~0.67),但整体证据指向中性结果。
全因住院率亦无显著差异(OR 0.97,0.83~1.14)。
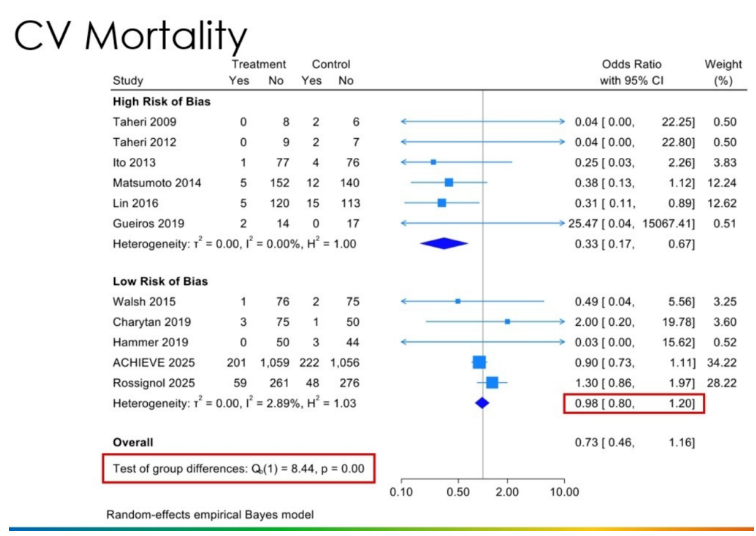
图1. 心血管死亡
2.心力衰竭住院:信号不确定
仅2项低偏倚研究分析显示,MRA组心力衰竭住院OR为0.70(0.30~1.65),但异质性较高(I2=71.1%),证据确定性低。
3.安全性问题:高钾血症与乳房不良反应突出
高钾血症(血钾≥6.5 mmol/L)风险增加50%(OR 1.50,1.11~2.03),绝对风险增加23/1000人。
男性乳房发育或乳房疼痛风险显著升高3.66倍(OR 3.66,1.82~7.36),绝对风险增加13/1000人。
低血压风险无显著变化(OR 1.04,0.61~1.78)。
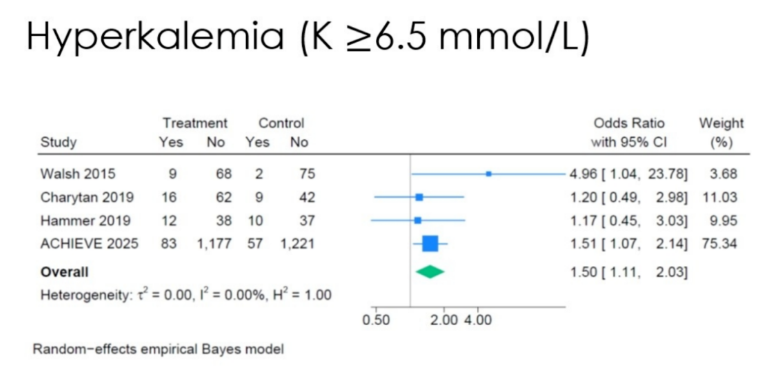
图2. 高钾血症情况
证据分级:中等确定性支持MRA的风险警示
GRADE评估显示,心血管死亡、全因死亡证据为中等确定性,高钾血症和乳房不良反应为中等确定性,心力衰竭住院为低确定性。研究指出,现有证据均来自甾体类MRA(如螺内酯、依普利酮),非甾体类MRA(如非奈利酮)在透析患者中的数据完全缺失。
肾医线:您的最新系统评价和荟萃分析聚焦于透析患者使用盐皮质激素受体拮抗剂的情况。从最新证据中,您观察到的最重要发现或趋势是什么?
Pyne博士:我们原本希望发现这类药物能降低心血管死亡率。但遗憾的是,与此前关于该主题的系统评价和荟萃分析结果相反,我们发现对于需要透析的肾衰竭患者,盐皮质激素受体拮抗剂并未降低心血管死亡风险,也未降低全因死亡率或心力衰竭住院率。从疗效来看,这类药物并无获益未显示出益处,反而带来了一些相关副作用,尤其是高钾血症发生率增加。我们将高钾血症定义为血钾≥6.5 mmol/L,其优势比约为1.5,即风险增加约50%;此外,男性乳房发育或乳房胀痛的发生率增加了3~3.5倍。而对于这一患者群体而言,盐皮质激素受体拮抗剂并未带来真正能抵消这些副作用的益处。
Nephrology On-line: Your updated systematic review and meta-analysis focus on mineralocorticoid receptor antagonists in dialysis patients. What are the most significant findings or trends you observed from the latest evidence?
Dr Pyne: We were hoping to find that they would lower cardiovascular mortality. Unfortunately, what we found was that in contrast to the prior systematic reviews and meta-analyses on this topic, mineralocorticoid receptor antagonists in patients with kidney failure requiring dialysis did not lower the rates of cardiovascular death, did not lower the rates of overall all-cause mortality, and did not lower the rates of heart failure hospitalization. So, in terms of efficacy, they were not found to be beneficial, and did have some relevant side effects, particularly increasing the rates of hyperkalemia. We defined hyperkalemia as potassium greater than or equal to 6.5. Odds ratio for that was about 1.5, so an approximately 50% increase, as well as a three to three-and-a-half times increase in the rate of gynecomastia or breast tenderness. So, some relevant side effects, but no really offsetting beneficial effects of mineralocorticoid receptor antagonists in this patient population.
肾医线:这些发现对当前肾衰竭透析患者的临床指南或治疗决策有何影响?
Pyne博士:至少在我的临床实践中,我并不会常规地对所有需要透析的终末期肾病患者使用盐皮质激素受体拮抗剂,临床实践指南中也未作此推荐。因此,这些发现与我的临床实践一致,即不常规推荐使用此类药物来降低心血管事件风险,同时也需考虑其显著的副作用。不过,对于存在其他适应证的患者(例如射血分数降低的心力衰竭患者),不应以此研究结果作为反对使用盐皮质激素受体拮抗剂的证据。这一结论仅针对未筛选的终末期肾病透析患者,我将继续保持不常规使用此类药物的临床实践。
Nephrology On-line: How do these findings influence current clinical guidelines or treatment decisions for patients with kidney failure on dialysis?
Dr Pyne: I think right now, at least in my own personal practice, I was not routinely using mineralocorticoid receptor antagonists for an unselected patient population with end-stage renal disease requiring dialysis, and nor was that something that was recommended in clinical practice guidelines. So, I think, in that sense, my own personal clinical practice would be pretty consistent, which is to say that they would not be recommended routinely to lower the risk of cardiovascular events, and also considering the important side effects profile there. Now, outside of that patient population, should they have another indication for mineralocorticoid receptor antagonists, if they have heart failure with reduced ejection fraction for example, I don't think this should be used as evidence to counteract that. This is merely saying, in an unselected patient population of end-stage renal disease requiring dialysis, I was not routinely using mineralocorticoid receptor antagonists and that will continue to be my practice.
肾医线:基于您的分析,该人群中盐皮质激素受体拮抗剂的安全性和有效性研究仍存在哪些空白?未来研究应优先关注哪些方向?
Pyne博士:我们的系统评价关注的是针对需要透析人群使用任何类型盐皮质激素受体拮抗剂(MRA)的随机对照试验。但我们发现,所有纳入的试验都仅使用了甾体类盐皮质激素受体拮抗剂。除了一项研究使用依普利酮外,其余均采用螺内酯 —— 这两种药物都属于甾体类 MRA。
在我看来,当前最明显的研究空白在于:非甾体类盐皮质激素受体拮抗剂的效果如何? 这类药物在透析患者中是否存在不同作用,是一个值得特别关注的领域。目前,至少在北美,可用的非甾体类MRA为非奈利酮,但它尚未获批用于需要透析的肾衰竭患者,这无疑是最关键的研究缺口之一。
此外,还有一些更重要的问题亟待解决:如何选择合适的临床终点?在需要透析的终末期肾病患者中,该如何定义 “心力衰竭住院”?我们是否需要对心血管终点进行更细致的分类?当前多数试验仅关注总体心血管死亡率,其中既包括心律失常、心源性猝死、心力衰竭等心脏事件,也混杂了心脏病发作、中风等血管事件。而 MRA 对这两类事件的影响是否存在差异,我认为值得深入探究。
Nephrology On-line: Based on your analysis, what are the remaining gaps in research regarding the safety and efficacy of mineralocorticoid receptor antagonists in this population, and what should future studies prioritize?
Dr Pyne: That's a great question. As mentioned, our systematic review was looking at randomized controlled trials of any type of mineralocorticoid receptor antagonists in people requiring dialysis. We only found trials using steroidal mineralocorticoid receptor antagonists. All of the studies, except for one, were of spironolactone. One was of eplerenone. Both spironolactone and eplerenone are steroidal mineralocorticoid receptor antagonists. So, to me, the most glaring gap would be what effect do non-steroidal mineralocorticoid receptor antagonists have? Whether or not there is a different effect in this patient population would be an area that I think would be of particular interest. Currently, at least in North America, the available non-steroidal mineralocorticoid receptor antagonist is finerenone but it is not approved for patients with kidney failure requiring dialysis. I think that would be one of the most relevant gaps. Then the bigger questions are what outcomes to use, how to define heart failure hospitalization in patients with end-stage disease requiring dialysis, and whether we need to be more narrow for our cardiovascular outcomes. Most of the trials looked at overall cardiovascular mortality, which includes cardiac events of arrhythmias and sudden cardiac death and heart failure, but also lumps vascular events in together, like heart attacks and strokes. Whether or not mineralocorticoid receptor antagonists affect those two types of events differently would, I think, be worth looking into.
报告概要
盐皮质激素受体拮抗剂在接受透析的肾衰竭患者中的应用:一项最新系统评价和荟萃分析
研究背景:透析患者心血管风险与MRA的应用争议
终末期肾病患者常伴随高发心血管事件,而盐皮质激素受体拮抗剂(MRAs)在慢性心力衰竭和慢性肾病(CKD)患者中已被证实可降低心血管风险。然而,这类药物在需要透析的肾衰竭患者中的疗效与安全性一直存在争议。
研究方法:纳入19项研究的全面证据整合
研究团队检索了截至2025年3月的MEDLINE、Embase等数据库,纳入19项随机对照试验(RCT),覆盖接受维持性透析(血液透析或腹膜透析)的成年患者,比较MRA(如螺内酯、依普利酮)与安慰剂/标准治疗的疗效与安全性。主要终点包括心血管死亡、心力衰竭住院、全因死亡,次要终点涉及高钾血症、男性乳房发育等不良反应。研究采用GRADE方法评估证据确定性,并通过随机效应模型分析异质性。
关键结果:MRA未带来生存获益,副作用显著
1.心血管与全因死亡无改善:
低偏倚风险研究显示,MRA组心血管死亡风险比(OR)为0.98(95%CI:0.80~1.20)(图1),全因死亡OR为0.97(0.84~1.21),均无统计学意义。高偏倚风险研究中,MRA虽显示心血管死亡风险降低(OR 0.33,0.17~0.67),但整体证据指向中性结果。
全因住院率亦无显著差异(OR 0.97,0.83~1.14)。

图1. 心血管死亡
2.心力衰竭住院:信号不确定
仅2项低偏倚研究分析显示,MRA组心力衰竭住院OR为0.70(0.30~1.65),但异质性较高(I2=71.1%),证据确定性低。
3.安全性问题:高钾血症与乳房不良反应突出
高钾血症(血钾≥6.5 mmol/L)风险增加50%(OR 1.50,1.11~2.03),绝对风险增加23/1000人。
男性乳房发育或乳房疼痛风险显著升高3.66倍(OR 3.66,1.82~7.36),绝对风险增加13/1000人。
低血压风险无显著变化(OR 1.04,0.61~1.78)。

图2. 高钾血症情况
证据分级:中等确定性支持MRA的风险警示
GRADE评估显示,心血管死亡、全因死亡证据为中等确定性,高钾血症和乳房不良反应为中等确定性,心力衰竭住院为低确定性。研究指出,现有证据均来自甾体类MRA(如螺内酯、依普利酮),非甾体类MRA(如非奈利酮)在透析患者中的数据完全缺失。
- 推荐文章
肾例明鉴 | 老年男性ANCA相关性血管炎伴口干、眼干:只是非特异性抗体阳性?还是重叠综合征?——1例病例报告并文献综述
恩格列净+非奈利酮联用,高钾血症风险几何?CONFIDENCE试验二次分析结果揭晓
人人享有肾脏健康:关爱生命,守护地球——2026年世界肾脏日公益活动举行
14:00直播!2026年世界肾脏日公益活动即将开始——人人享有肾脏健康:关爱生命,守护地球
血液透析的环境挑战与可持续发展路径探索——2026世界肾脏日特别关注
特别策划 | 世界肾脏日:您真的了解肾脏健康吗?
肾域华章 | 儿童增殖性狼疮肾炎初始治疗添安全新选:多中心RCT证实吗替麦考酚酯非劣效于环磷酰胺选
2026世界肾脏日 | 绿色肾移植十策:让肾移植告别等待,共护双肾与地球
靶向清除“僵尸细胞”,达沙替尼联合槲皮素为糖尿病肾病治疗开辟新路径
慢性肾脏病与认知障碍:肾病越重,认知风险越高?——基于CRIC研究的新发现
膜性肾病精准诊疗的新证据:生物标志物和临床病理特征研究进展
eGFR百分位数:CKD早期识别的个性化新工具
PI解读:FSGS治疗新曙光——靶向药物迎来突破性进展
突破性进展:靶向补体因子B的RNA疗法为IgA肾病治疗带来新希望
利妥昔单抗血药浓度:膜性肾病早期治疗反应的预测标志物
肾例明鉴|43岁男子双下肢水肿、肌酐飙升,背后竟是两种肾病罕见叠加作祟!膜性肾病合并抗GBM病该如何破局?
Richard Lafayette教授:新型补体抑制剂时代下荚膜菌感染的防控指南
孙英贤教授牵头多中心研究:CRHCP事后分析揭秘CKM综合征不同分期强化降压价值
肾识百科|娃的肾病竟是遗传的?6种遗传性肾病家长必知!
护肾先护肠?1.2万人的迄今最大研究发现:肠道菌群及其代谢产物参与肾功能早期变化
肥胖与慢性肾脏病:不可忽视的“代谢多米诺”
《柳叶刀》:TRPC6抑制剂BI 764198治疗FSGS的Ⅱ期临床试验取得积极结果,为其足细胞靶向治疗提供首个有效证据
长期血透别忽视疼痛!平均8个部位受累,84%病程超1年、75%每日受折磨,肌肉骨骼和神经病理性痛为主要类型
近16万人数据:这样吃,大脑更年轻
美国麻省总医院最新综述:CKD-aP的诊疗进展与未来方向
超88%患者未获诊疗!Ⅲ期研究首证中国血透CKD-aP人群可从Difelikefalin治疗中获益
睡不好,血糖更难控?最新研究揭示:睡眠障碍正在悄悄扰乱你的“升糖”与“降糖”激素!
KDIGO肾小球疾病指南工作组主席Jürgen Floege教授:补体旁路途径是驱动CMKDs肾小球炎症的核心引擎
沉默的神偷!无声无息偷走小孩子肾脏功能的遗传性肾病——Dent病
国际组织在行动:CKM综合征、新型超级专科与“关爱肾脏”倡议
白蛋白尿——盐皮质激素受体拮抗剂带来肾脏获益的核心驱动因素
补体靶向时代:IgA肾病新疗法的疗效排名与精准化探索
从认知到实践:中国肾脏科医生IgA肾病诊疗现状与差距
肾例明鉴丨年轻痛风不是小事!19岁小伙关节痛3年,没控尿酸把肾“熬”成慢性肾病Ⅲ期
尿酸与非酒精性脂肪肝的“隐秘关联”:高血压人群需警惕的代谢信号
狼疮肾炎患者妊娠:她安然度过,她产后风暴骤起——来自两个临床病例研究的启示
罕见的先天性肾脏发育不良疾病——肾小球巨大而又稀少的“寡巨肾”,你听说过吗?
阿塞西普:IgA肾病治疗的新曙光——ORIGIN 3试验中期数据深度剖析
生殖史如何塑造年轻女性的心肾代谢风险?
指南共识丨《IgA肾病临床实践60问(2026版)》核心要点与临床实践解读(附原文)
司美格鲁肽获批治疗2型糖尿病合并慢性肾脏病1周年:糖尿病、肾脏与心脏疾病领域的变革
佳节健康“喝”出来——咖啡与茶,提神背后的健康双面性
春节期间重磅新闻速递:膜性肾病、IgA肾病、卵巢功能早衰领域迎来治疗新进展
“钾”在悄悄溜走,肾脏在喊“救命”!一种罕见的遗传性失盐性肾小管疾病
冬季假期真的会“悄悄让人发胖”吗?
肾友过年“四大护法”!作息·出行·娱乐·情绪,这份春节健康手册请收好
新春护肾,安心团圆:肾友及四高人群春节健康全攻略
学术纵横|多维靶向,精准护肾:小干扰RNA、ASI、nsMRA、GLP-1RA等新型药物均可为CKD患者保驾护航
尿糖阳性=糖尿病?那可不一定!这种罕见肾病会遗传尿糖,别当成普通糖尿病来治
聚焦CKM综合管理,恒格列净相关复方制剂赋能心-肾-代谢多重获益
年度盘点丨周晓玲教授:肥胖相关慢性肾脏病的诊治进展
肾例明鉴丨服药后肺肾接连“报警”!20岁女生的惊魂经历:元凶竟是治疗甲亢的丙硫氧嘧啶
谨慎“跟风养生”!Omega-3、生酮饮食、禁糖等营养宣传需辩证对待
肾识百科丨肾友想生娃?4类可怀情况 + 3类禁忌,提前看清不踩坑
警惕身体的“代谢紊乱风暴”!代谢综合征——引人关注的肾脏“杀手”
